Plantar fasciitis results in widespread discomfort because the plantar fascia located at the foot bottom becomes inflamed. The condition impacts people who maintain standing positions or walk and run at length. The condition has the ability to degrade performance when left without treatment. This article examines the fundamental sources of plantar fasciitis together with its risk variables followed by effective prevention methods and therapeutic approaches which will enhance your ability to handle this condition.
Understanding the Anatomy of the Foot

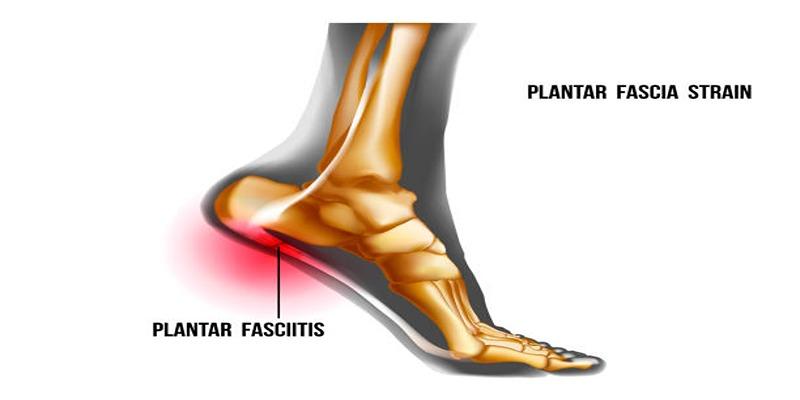
Knowledge about foot anatomy serves as a foundation to examine the fundamental underlying reasons behind plantar fasciitis development. Your heel bone meets your toes through the thick plantar fascia tissue structure which provides support to your foot arch.
The foot benefits from the protective role of this structure since it spreads out body weight when someone walks or runs. The plantar fascia develops pain through small tissue tears which appear when pressure or strain exceeds its tolerance.
7 Causes of Plantar Fasciitis
Understanding the factors that contribute to plantar fasciitis can help in managing and preventing this condition effectively. Below are seven common causes of plantar fasciitis:
1.Overuse or Repetitive Strain
Plantar fasciitis is a common condition caused by repetitive strain on the feet from activities like running, walking, or standing for long periods. This strain affects the plantar fascia, a thick band of tissue along the bottom of your foot that connects the heel to the toes and supports the foot's arch. Over time, repeated stress can cause small tears, leading to inflammation and heel pain, often felt most in the morning or after resting.
Athletes, especially runners, and people with jobs that require long hours of standing, like healthcare workers or retail employees, are at higher risk. Factors like unsupportive footwear, excess weight, or foot mechanics such as high arches or flat feet can increase the likelihood of the condition.
2.Tight Calf Muscles
Tight calf muscles can contribute to plantar fasciitis by pulling on your Achilles tendon, which connects the calf muscles to the heel bone. This added tension increases stress on the plantar fascia, leading to discomfort and inflammation.
Stretching your calf muscles regularly can help prevent these issues. Calf stretches, such as wall stretches or heel drops, improve flexibility and reduce strain. Properly warming up before exercise and maintaining a consistent stretching routine can make a significant difference in protecting your plantar fascia.
3.Flat Feet or High Arches
Flat feet and high arches are both common factors that can increase the risk of plantar fasciitis. Flat feet often lead to overpronation, causing the feet to roll inward excessively and creating uneven weight distribution. In contrast, high arches focus pressure on the heel and ball of the foot.
Both conditions place extra strain on the plantar fascia, leading to inflammation and pain. To prevent plantar fasciitis, consider wearing well-cushioned, supportive shoes or using orthotic inserts to evenly distribute pressure and alleviate stress on the foot.
4.Improper Footwear
Wearing shoes without proper arch support or with worn-out soles can contribute to plantar fasciitis. Unsupportive footwear fails to distribute weight evenly across your feet, putting excess strain on the plantar fascia.
High heels, flip-flops, and unsupportive flats are common culprits. Choosing shoes with good arch support, a cushioned sole, and proper fit can help prevent heel pain. Replace old or worn-out shoes regularly, especially if you use them for sports or prolonged walking.
5.Obesity
Excess weight places additional pressure on your feet, particularly the plantar fascia, which absorbs much of the impact as you walk or stand. Over time, this pressure can lead to inflammation and small tears in the tissue, causing plantar fasciitis.
Weight management through a balanced diet and regular low-impact exercises, like swimming or cycling, can reduce the strain on your feet. Supporting your weight loss journey with proper footwear can also alleviate stress on the plantar fascia.
6.Age
As we age, the body's natural healing ability weakens, making it harder for the plantar fascia to recover from strain or injury. Additionally, the padding on the soles of the feet thins over time, reducing shock absorption and increasing the chance of developing plantar fasciitis.
Older individuals should prioritize supportive footwear and regular stretching exercises to maintain foot health. Taking proactive measures, like strengthening foot and calf muscles, can help prevent plantar fasciitis-related issues in later years.
7.Medical Conditions
Certain medical conditions, like arthritis, diabetes, and nerve damage, can increase the risk of plantar fasciitis. Rheumatoid arthritis causes joint inflammation that can spread to the plantar fascia, leading to pain and stiffness. Diabetes often results in poor circulation and slower healing, making foot injuries harder to recover from.
It can also cause neuropathy, reducing foot sensation and awareness of early pain or damage. Nerve damage from diabetes, injury, or other issues can change how a person walks or stands, adding strain to the plantar fascia.
Strategies for Prevention and Treatment
While there is no one-size-fits-all solution for preventing or treating plantar fasciitis, the following strategies can help manage and alleviate symptoms:
- Rest: If you experience heel pain, take a break from activities that aggravate it. Avoid high-impact exercises and opt for low-impact alternatives like swimming or cycling.
- Stretching: Regularly stretching your calf muscles and feet can help prevent strain on the plantar fascia. Consult with a physical therapist to learn proper stretching techniques.
- Supportive footwear: Choose shoes with good arch support, cushioned soles, and proper fit to reduce pressure on the plantar fascia. Consider using orthotic inserts for added support.
- Ice therapy: Applying ice to the affected area can help reduce inflammation and pain. Use an ice pack or a frozen water bottle for 15-20 minutes at a time, several times a day.
- Medical treatments: In severe cases, doctors may recommend physical therapy, corticosteroid injections, or shockwave therapy to manage symptoms. Surgery is rarely necessary.
- Preventative measures: If you are at risk for plantar fasciitis due to factors like age, weight, or medical conditions, take proactive steps to maintain foot health.
Conclusion
Plantar fasciitis can be a painful and disruptive condition, but with proper care and preventative measures, its impact can be minimized. By incorporating stretching routines, wearing supportive footwear, and exploring treatment options when necessary, individuals can manage symptoms effectively and prevent recurrence. Early intervention is key to avoiding complications, so it is essential to listen to your body and seek professional advice if pain persists. Prioritizing foot health not only alleviates current discomfort but also contributes to overall physical well-being, enabling you to stay active and enjoy a better quality of life.










